Introduction
There have been many complaints about prescription drug prices lately; critics seem to think they are too high, and point to drug company profits as proof.
In an effort to lower drug prices, many critics are looking for ways to impose price controls on prescription drugs. For example, on June 27, some 20 states plus the AFL-CIO and a number of liberal advocacy groups gathered both in Washington and at several state houses around the country in a show of support for pharmaceutical price control legislation that has already been passed in Maine. Participants claimed to “recognize that prescription drug prices are spiraling out of control,” and they intended to do something about it.
But would imposing price controls on drugs be good policy for the public, states and the nation? Would there be unintended consequences? Would such policies reduce or eliminate drug manufacturers’ research and development efforts? Are there deadly or debilitating diseases that won’t be treated or cured if price controls are implemented? How many people would die for lack of a new drug that might have been developed had price controls never been adopted?
Like most decisions in life, public policy proposals involve trade-offs. While price-control advocates are good at recognizing the high cost of a drug, they never take time to count the high cost of not having it. A government decision to make prescription drugs more “affordable” by imposing price controls would mean less money available for research and development. At that point, Who will be cured?, What will be cured?, and, When will it be cured?, become political questions, not technological ones. Money will be saved, but lives will be lost. Will it be worth it? Probably not if you are one of those who needs the drug that was never invented.
Does that mean that public policy can do nothing in the face of rising drug costs? No. There are two ways to hold down drug prices: government-imposed price controls or competition. Increased competition spurs manufacturers to create better products at lower prices, even when the competitors have a copyright or a patent. When competition, rather than government, forces manufacturers to hold prices down, they look for innovative ways to cut their costs and still deliver a quality product. When government forces companies to hold their prices down, they look for lobbyists to help them carve out exceptions and special consideration.
If Congress wants to lower drug prices, there’s a right and a wrong way to do it. Government almost always picks the wrong way; this paper outlines the right way.
Are Prescription Drugs Expensive?
Some drugs are very expensive, others aren’t. What’s the difference? Research and development. As Figure 1 shows, pharmaceutical companies will spend about $22.4 billion in 2000 developing and testing new drugs, as compared to about $4 billion for all other countries combined.1 Drug companies have to recover those costs if they intend to continue that R & D.
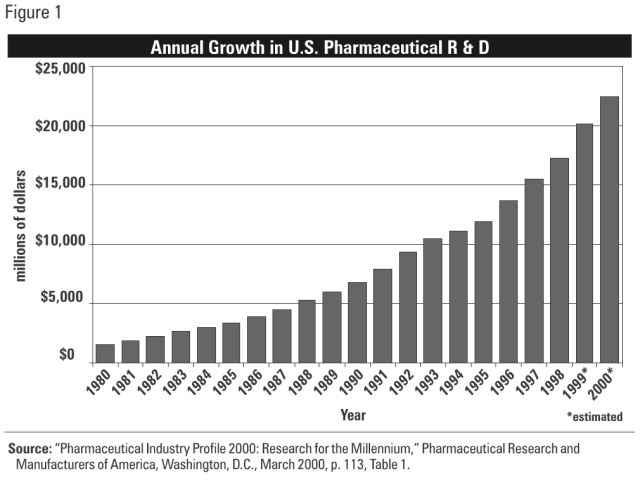
Pharmaceuticals in the New Economy.
Not all drugs are expensive; most over-the-counter drugs are very affordable, which highlights an important distinction. There are really two pharmaceutical industries: one that mass produces aspirin, cold medicines, ointments and other over-the-counter (OTC) drugs and one that spends billions of dollars each year creating and developing new prescription drugs that relieve pain, cure disease and save lives. The OTC market fits nicely in an Old Economy model where there are some research costs, but competition is high and prices are low.
The other pharmaceutical industry — the “pharmatech” industry — is a New Economy industry, where initial costs to create and test a patentable item are very high, but once achieved the reproduction costs are usually minimal.
In the Old Economy model, the barrier for competitors is the ability to produce a service or product similar to that of a successful company, but at a lower price. For a New Economy company, the primary barrier is the cost of developing the intellectual property, which may be patented in order to protect the monopoly.
Treasury Secretary Lawrence Summers understands this principle well. In a speech delivered in May in San Francisco, Summers said that at the heart of this thing called the New Economy “must be the move from an economy based on the production of physical goods to an economy based on the production and application of knowledge” — or what he calls “knowledge goods.”2 Thus, “An information-based world is one in which more of the goods that are produced will have the character of pharmaceuticals or books or records, in that they involve very large fixed costs and much smaller marginal costs.”3 And that change bears significantly on the nature of economic incentives. According to Summers, in an information-based economy, “the only incentive to produce anything is possession of temporary monopoly power — because without that power the price will be bid down to the marginal cost, and the high initial fixed costs cannot be recouped.”4
Recovering Research and Development Costs.
Since, as Secretary Summers suggests, the pharmatech industry’s need for temporary monopoly profits is an inherent function of a high-tech industry in an information- based economy, then attempting to restrain or undermine that quest could mean the death of the industry. Yet recovering those costs can make prescription drugs expensive. Just consider:
- Suppose it takes $500 million (the number usually cited as the average cost to develop a new drug) to develop a new pain pill.5
- At $2 a pill — roughly $60 for a month’s prescription — a drug company would have to sell 250 million pills just to recover its research costs.
- That works out to nearly 140,000 people taking one pill a day for five years just to break even — and that’s before the pharmacy marks up the price or the manufacturer makes a profit.
Some of the new specialty drugs that target uncommon diseases, and are therefore spread out over relatively few people, will have to cost a lot more. Clearly, we are entering a period where more and more drugs will be available, but some of them won’t be cheap.
Why Drug Companies Are Profitable
It is true that most pharmaceutical companies are profitable — with median profits about 18 percent of revenue in 1999, according to Fortune magazine. Some critics cite those profits as evidence that drug companies are price gouging. The real issue is whether drug company profits are comparable with other New Economy, or even some Old Economy, companies.
What We Need Is a Cheaper Coca-Cola.
Table 1 tracks profits as a percent of revenues for several companies over the past decade as compared to the median profit of several pharmaceutical companies. According to the figure:6
- Coca-Cola frequently showed higher profits than the pharmatech industry.
- And Microsoft had significantly higher profits, while Oracle was only slightly below the pharmatech median.
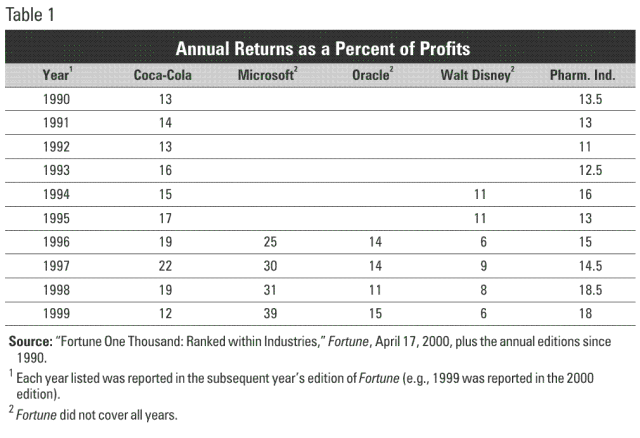
Moreover, as shown in Figure 2, a number of industries had median profits very close to the pharmaceutical industry’s.
While it is true that many prescription drug manufacturers are profitable, and several have been consistently profitable over the years, those profits are not out of line with other successful New Economy companies and industries, and even some Old Economy companies, that deal in intellectual property or other patentable or copyrighted products.
Say, Buddy, Can You Spare a Big Mac?
One of the primary criticisms is that drug companies charge Americans too much for their drugs. As a result, critics claim, thousands of Americans cross both the Canadian and Mexican borders to buy cheaper prescription drugs.
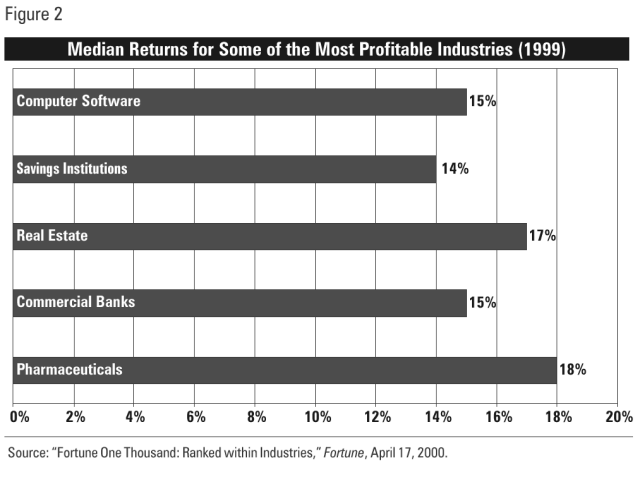
While some drugs are more expensive in the U.S., others are cheaper. The cost of a drug, both here and abroad, depends on a number of factors — just like the price of other items, such as food. For example, look at the price of a McDonald’s Big Mac. As Figure 3 shows, the price of a Big Mac can vary from country to country — and the U.S. is by no means the most expensive.
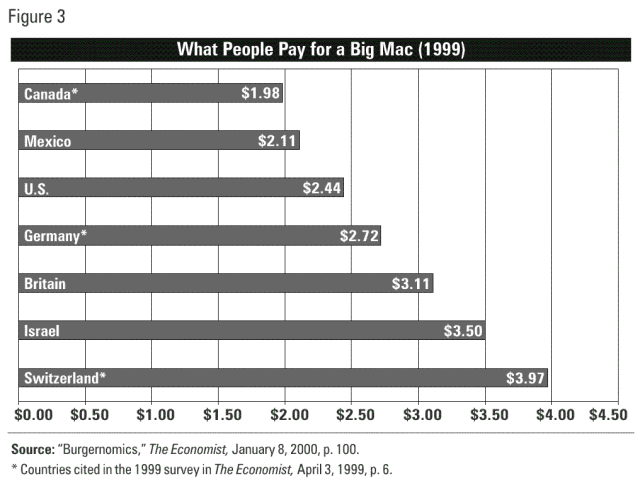
In light of these numbers, there is a real possibility that seniors in need of an affordable lunch at McDonald’s are crossing the border from Switzerland into Germany. And look for U.S. lawmakers to propose legislation that would ensure that Americans get as good a deal on a Big Mac as our Canadian counterparts.
The point is that drug prices will vary by country, based on a number of factors, just as many other products will. However, those differences have been vastly exaggerated by critics of the drug industry. A now well-known April 1999 comparison of drug costs in several countries by Prof. Patricia M. Danzon of the University of Pennsylvania’s Wharton School of Business found that “Canadian prices are between 13 percent lower and 3 percent higher than the U.S., depending on the price index used.”7
People Want What Drug Companies Sell.
Which brings us to an important point: drug companies are not profitable because they charge so much for many prescriptions; they are profitable because they produce products that doctors and their patients want. However, while a company like Coca-Cola stays profitable by promoting the same product year after year, pharmaceutical and computer software companies make their money by continually releasing new or upgraded products.
As a result, while total spending on pharmaceuticals has been growing rapidly — averaging a 13.7 percent annual increase between 1995 and 1999 — most of that spending is due to increased volume of sales, not higher prices.8 For example, while prescription drug sales grew by 18.8 percent in 1999, 14.6 percentage points of that growth was due to increased volume and new products, while only 4.2 percentage points of the increase was due to higher prices. [See Table 2.]
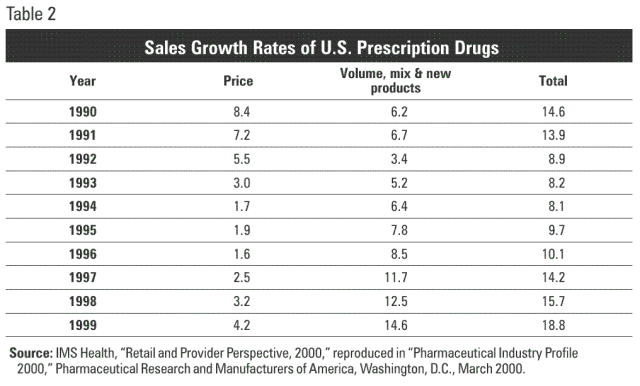
Several members of Congress and the state legislatures have expressed support for price controls on pharmaceuticals as a way to keep costs down. But since most of the increase in total prescription drug spending comes as a result of increased utilization, imposing price controls would have little impact on total drug spending.
Do Price Controls Work?
Interestingly, Congress already has had some experience with trying to control rapidly rising health care costs — in the Medicare program. Concerned about an explosion of spending in Medicare in the 1980s, Congress imposed price controls on hospitals through a process known as Diagnosis Related Groups (DRGs). Hospitals receive a specific amount of Medicare reimbursement money for each patient based on the diagnosis. Later, a similar program was established for physicians. Did DRGs control Medicare costs? No, many hospitals, and later doctors, when faced with a similar situation, simply increased their volume or made more per procedure by “upcoding,” using a diagnosis that was still compatible with the symptoms but would draw a higher reimbursement rate.
This is not to suggest that the pharmaceutical industry would or could adopt such practices, nor that the practice is always and necessarily a result of fraud. Hospital billing procedures remain a mystery to most people, making it possible to maximize revenue in a price-controlled system. It is simply to demonstrate that price controls do not work. There is a real danger that uninformed or politically pressured lawmakers both at the state and federal levels will look at total prescription drug spending, assume it’s a result of price gouging, and try to impose price controls.
When Did We Start Punishing Success?
Such a practice would only be punishing success. What the pharmaceutical industry appears to have done better than most is to find products that doctors and patients want and are willing to pay for — or, at least, have a third party pay for. As a result, patients, their doctors, their loved ones and the pharmaceutical companies have benefitted.
So why would politicians both at the federal and state levels feel compelled to insert themselves in the middle of this American success story? Votes, in most cases. Critics of the pharmatech industry like to portray it as a for-profit industry taking advantage of the old and the poor who need their products. By trumping up a crisis mentality that says millions of seniors are going without food in order to buy their prescription drugs, lawmakers, along with several advocacy groups, are attempting to create the political pressure for Congress to act.
Do Seniors Need a Prescription Drug Benefit?
Currently, about 65 percent of seniors have some type of coverage for prescription drugs.9
- 28 percent receive that coverage through a former employer;
- 11 percent were considered poor enough to receive Medicaid coverage for their prescription drugs;
- And 15 percent purchased their own supplemental policies or received their coverage through a Medicare HMO.
Of the 35 percent who do not have coverage, many of them are healthy and face relatively low expenses. Most have made a conscious decision — which may be reasonable given the fact that they are healthy — not to purchase drug coverage. In other words, just because 35 percent of seniors don’t have supplemental coverage doesn’t mean they have serious health care problems or high drug expenses. Some do, but most don’t. However, some who don’t have coverage — and even those seniors who have limited drug benefits — can face some very high drug bills should a major accident or illness arise.
This fact underlies one of the perverse incentives in the structure of the Medicare program: it covers some therapies, such as surgery, but not prescription drugs, which in many cases might be cheaper, less invasive, safer and more efficacious. That means that for some diseases and for some patients, Medicare may be spending more than it would if the program had a prescription drug benefit.
The Republican and Democratic Proposals.
To address this problem, both Democrats and Republicans have proposed prescription drug benefit legislation meant to help up to 39 million mostly seniors on Medicare get the prescription drugs they need. While the Republican bill is better than the Democratic version, both have their problems.
On the plus side, the Republican plan tries to lure private-sector insurers into providing seniors with a prescription drug benefit. Seniors would pay about $40 in monthly premiums, plus a deductible of $250 a year. After the deductible was met, insurance would pay half the cost of prescription drugs up to a total of $2,100. There is also a catastrophic provision that would pay most costs after $6,000 in drug expenses.
The Democratic plan differs little in the specifics. It would only charge $25 a month in premium initially, and would pay half of all prescription drug costs from the first dollar (i.e., there is no deductible), up to a total of $2,000 a year (half paid by the patient and half by the government, just as in the Republican plan). Premiums would rise over several years to around $48 a month, but so would the coverage — up to $5,000 ($2,500 each from the senior and the government). Total out-of-pocket expenses would be capped at $4,000.
While the mechanics of both plans are similar, the philosophy underlying them is very different. The Democratic plan creates a new Medicare entitlement at a time when the program is already facing serious funding problems in the near future. In addition, the government will know what drugs seniors are using because it will be paying half of the bill, which raises some serious privacy concerns. Finally, the plan treats lower-income and wealthy seniors the same by paying for drugs that many seniors are able to pay for out-of-pocket.
Proponents of the Democratic plan assert that theirs is not a new entitlement program because it is voluntary and that price controls are not part of the legislation. But Medicare certainly is an entitlement, yet Medicare Part B, the program that pays for physician and outpatient services, also is voluntary and charges a monthly premium — just like the prescription drug benefit proposal. In addition, price controls played no role in the passage of Medicare. In fact, price controls would have killed the legislation. Medicare opponents demanded that the legislation guarantee that doctors could charge their “reasonable and customary” fees or it never would have passed. Yet today, both Medicare Part A and B operate under price controls. Drug benefit proponents should learn from history: even a guarantee that there will be no price controls imposed on prescription drugs can be set aside whenever Congress chooses to do so.
The Republican plan, by contrast, turns to private insurers to provide the drug benefit in an effort to ensure seniors’ privacy from government intrusion. It therefore keeps information about which drugs seniors are using out of the hands of bureaucrats. However, insurers are not going to be able to handle the drug benefit plan financially, even with subsidies from the federal government, and they have already expressed a reluctance to participate.
Can Their Proposals Work?
Is this a reasonable approach to providing prescription drug coverage? Well, consider that the average senior spends about $600 a year on prescription drugs.10 Under the Democratic plan, a senior would pay half of that, or $300, while the government would pay the other half. However, since the Democrats would charge $25 a month to be enrolled, or $300 a year, a senior who has the average annual drug costs would be no better off with the Democratic version, because he would have spent $600 either way.
Thus the Democratic plan might work actuarially, but only if it had a representative share of the sick and healthy enrolled. That won’t happen. In fact, since both the Democrats and the Republicans make their plans voluntary, seniors will calculate their costs — or expected costs — and ask themselves whether they would be better off in the plan or out of it. Those with employer-provided policies that cover what Medicare doesn’t will likely stay with their employer-provided coverage. Those who purchase their own supplemental drug coverage will make comparisons and see which plan would be better for them. Finally, those with no coverage but low drug costs (i.e., they’re healthy) may choose to stay out.
What that means is that the Democratic plan would cause rampant “adverse selection” — the situation where a disproportionate number of sick people join a plan. When that occurs, the $25-a-month premium won’t be nearly enough, especially as seniors begin to consume both more drugs and more expensive drugs because they are insulated from the full price. That’s the primary reason why the Democratic plan is projected to cost about $200 billion over 10 years ($253 billion under President Clinton’s proposal). The Republican plan will likely also lead to adverse selection, but they charge a higher premium to help cover the costs.
Would Seniors Join the Plan?
Would either of these proposals be a good deal for seniors? Not for Mary Valentine. Mary, a widow in her 70s living in a suburb north of Dallas, already has prescription drug coverage. It’s part of a retirement plan she has from where her late husband retired.
Mary has something else: drug bills. Her three prescriptions cost about $190 a month. Her retirement plan requires a co-payment of only $3 per prescription, for a total of $9 a month out of her own pocket. Under the Democratic plan, she would have to pay a $25 per-month premium, plus $95 a month out of her own pocket in copayments, for a total of $120 a month. And because in her case the Democratic plan would hit its cap after about 10 months, Mary would have to pay all expenses plus the premium for the last two months. Of course, Mary would face an even worse deal under the Republican proposal.
The Democrats’ plan would also be a bad deal for Don and Rubee Parlett of Phoenix, Arizona. Don, now in his early 70s, retired nine years ago. He was one of those able to take early retirement, in part because his employer provided him with health insurance, which now only pays for what Medicare doesn’t cover, like prescription drugs.
Don and Rubee take about nine prescriptions a month between the two of them, costing an estimated $400 a month. Since there is a $7 per-prescription copayment, they spend a little more than $60 a month out of their own pocket — with the employer-provided drug benefit paying the rest.
How would the Parletts do under the drug benefit plans? Well, to begin with they would both have to pay the $25 per-month premium under the Democrats’ plan. And instead of $60 a month out of pocket, they would be looking at about $200, with the plan paying the other $200 until they reached the cap, which would come in about five months. And again, they would be even worse off under the Republican plan. So don’t expect the Parletts to be first in line to sign up for the prescription drug benefit.
So who would join? Those with moderate or heavy drug costs, which means the plan would attract a disproportionate number of sick people. While drug benefit proponents might point out that the legislation attempts to minimize adverse selection by limiting when seniors can join, those limits would be soon discarded. For years several members of Congress have tried to coax or force health insurers and those companies that provide Medicare supplemental (medigap) coverage into accepting anyone regardless of health status. It certainly wouldn’t be long before Congress would impose this rule on its own plan. As more and more of the sick entered the plan, costs would begin to rise rapidly, and that’s when Congress would feel compelled to step into the middle of it.
Would the Plan Lead to Price Controls?
While paying for those drugs might not be difficult in a time of budget surpluses, what happens if there is an economic downturn? Congress, faced with rising drug costs and utilization, would look for ways to cut back — just as it did to Medicare in 1997. Congress might try to impose price controls on the pharmaceutical industry, limit the availability of certain drugs, raise premiums or cut benefits — or some combination of all of the above.
How can we know this would be the legislative response? We have plenty of evidence both from here and other countries that already have price controls.
Congress and the Health Care Financing Administration (HCFA) control how much the federal government will spend for seniors on Medicare HMOs. The managed care industry is estimating that some 1.7 million seniors will lose their Medicare HMO coverage by the end of 2000, and many others will have to pay more for the HMO coverage they receive.11 The reason? Money. As part of the Balanced Budget Act of 1997, Congress cut back significantly on Medicare HMO and home health care payments. As a result, hundreds of thousands of seniors have seen their HMO benefits reduced — including their prescription drug benefit — or canceled all together. While Congress has stepped in with additional funding, and may do so again, it has not been enough to stem the exodus. The great irony here is that while several members of Congress demagogue about seniors’ need for a prescription drug benefit, Congress has done more than anyone to cause seniors to lose their coverage.
Moreover, governments in Europe routinely delay access to new drugs, limit their availability by imposing tight prescribing restrictions or simply refuse to pay for them.12 Ironically, it’s these other countries where prescription drug rationing is blatant and unapologetic that some drug benefit proponents point to as models for the U.S. to follow.
Would the Quality of Care Decline?
But there is another problem: quality of care. When Congress cuts reimbursement rates below a certain level, health care quality will begin to decline. What would that mean for prescription drugs? It could mean limiting access to only the least expensive drugs for a specific medical condition, even if a more expensive drug would be more efficacious.
Remember, once Congress creates a prescription drug benefit, entry into the program and what the program provides are political questions, not business or actuarial questions. There will be tremendous pressure on Congress to let the sick in when they want in, and that will discourage the healthy from signing up until they need the benefit. There will also be pressure on Congress to hold down costs, and that will eventually limit choice and reduce the quality of care.
The Role of Competition in Real Markets
If politicians really want to control prescription drug prices, there is a better way to do it than by government fiat. It’s called competition. In fact, that remedy may already be taking effect — if politicians will leave their hands off long enough for the market to work.
In a real market:
- Companies create products they think will sell and then advertise in order to attract customers and maximize sales. That is what is beginning to happen in the pharmaceutical industry, as companies increasingly target consumers with their drug ads.
- When a company is successful in attracting customers to its new products, profits may go up — which in turn attracts competitors to enter the market with the same or a similar product. When a company has the corner on a market, often because of a copyright or patent, economists call it “monopoly profits.” If competitors are prohibited by copyright or patent laws from duplicating the product, they often try to come up with knock-offs or substitutes in the hope of attracting some of those consumer dollars.
- Once competition sets in, companies begin to look for ways to maintain a certain share of the market. They may cut prices, advertise more or engage in other activities intended to attract more consumers.
- If competitors are successful, the sales and prices of the first company will begin to decline, which may also reduce profits.
Economists know this pattern well and usually argue that it is best to let the process work. The lure of profits is what drives a company to come up with a new product in the first place, and it’s the lure of profits that drive other companies to imitate a product when one company is successful. Thus, a new idea or product may make lots of money for a little while, but competition eventually reverses that situation.
Can Prescription Drugs Constitute a Real Market?
But can prescription drugs, many of which are protected by a patent, act like a market? Yes, competition can even force monopoly prices somewhat lower when there are numerous similar competing products.
Take Coca-Cola, for example. Even though it is one of the most recognized products in the world, it must remain competitive on its price or people both here and abroad will switch to a competing soft drink. Yet even under very competitive pricing, Coca-Cola manages to remain one of Fortune magazine’s most profitable companies.
The Drug Industry Is Already Competitive.
The drug industry is also very competitive. No drug company has more than 7.2 percent of the market.13 And changes in the health care system and with patients’ ability to access information are making the market even more competitive.
Take direct-to-consumer (DTC) advertising, for example. Congress has already adopted some policies that have enhanced competition among drug companies, which explains their heightened visibility. In just 10 years DTC advertising has increased from $55 million (1991) to an estimated $1.8 billion this year. However, most of that growth came after 1997, when the Food and Drug Administration (FDA) loosened some of the restrictions on DTC ads.14 For example:
- In the first half of 1998, pharmaceutical marketers spent $273.3 million on DTC television ads, an increase of 312.5 percent over the same period in 1997.
- While drug companies spent 19.6 percent of their total DTC dollars on TV ads in the first half of 1997, they spent 47.7 percent in the first half of 1998.
And those ads have had an impact on consumer behavior. Prior to the change in guidelines, 41 percent of the physicians surveyed by IMS Health said they had observed an increase in patients’ requests for brand name drugs. After the change, 65 percent of the physicians surveyed noticed an increase in brand-name requests.15
While increased advertising expands information and enhances brand recognition, it doesn’t necessarily increase competition. If there is only one product treating a specific illness or medical condition, the manufacturer can still make monopoly profits. However, manufacturers have to be more cautious about pricing when there are competing products. Fortunately, many medical conditions are being treated with a growing number of products.
For example, in the first half of 1998, drug companies advertised 74 different prescription drug products in the DTC market. However, not all drugs are advertised equally. Schering-Plough spent about $58 million advertising its allergy drug Claritin in the first half of 1998.16 When ranked by the amount spent on advertising a drug, that was equal to the total spent on the bottom 52 drugs. One reason for that decision to advertise so extensively may be the competition: in the top 20 advertised drugs, there are four targeting allergies: Claritin, Zyrtec, Allegra and Flonase, and all four come from different manufactures. [See Table 3.]
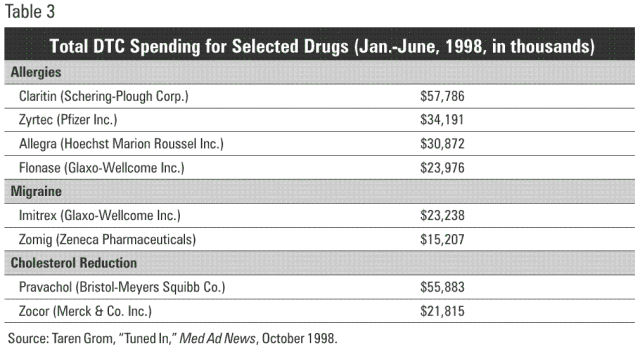
The explosion in pharmaceutical R & D has led different companies to create different patentable products for the same condition. For example, there are three “superaspirins” — Arthrotec, Vioxx and Celebrex — currently on the market for treating chronic pain such as arthritis. All three cost about the same, around $75 to $80 per month. In an increasingly competitive market, you would expect one company, trying to gain market share, to lower its price to attract more customers.
It seems clear from the amount of money being spent that the pharmatech industry is getting more competitive as companies vie for market share. Will that competition eventually lead to lower prices? That’s what would happen in a real market.
Limits to a Prescription Drug Market.
True, the prescription drug market doesn’t work exactly like a normal market for three reasons:
- Patents create a barrier to entry. But, as has been pointed out, drug companies are still free to develop different drugs that treat the same disease or medical condition.
- A physician who doesn’t have to pay for the drug fills out the prescription for a patient who does. But many physicians are sensitive to costs and want to prescribe the product with the best effect at the lowest cost, and they are increasingly willing to make cost considerations a factor.
- Most patients have insurance that insulates them from the price of prescription drugs, which means they are not price sensitive. As a result, they want the best drug available, irrespective of the price.
Limited Competition vs. Perfect Competition.
Economic theory tells us that in a state of “perfect competition” prices tend to drop until the price equals the cost of production. And while perfect competition never really exists because there are always some distorting factors, many industries come closer to that condition than the pharmaceutical industry. In those industries, prices tend to be very low, and so do profits.
For example, while the computer software industry, which has copyright protection on its intellectual property, had a median profit of about 15 percent in 1999, according to Fortune, the computer hardware industry claimed only about 7 percent. As Table 4 shows, some of the most competitive industries have relatively low profits.
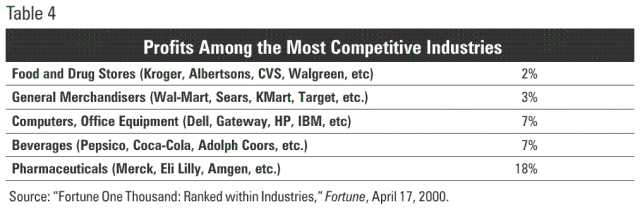
Each of the lower-profit industries advertise heavily and compete on prices. And even though some companies within a given industry are very profitable (e.g., Coca-Cola), overall profits remain low in part because competition is so stiff.
The pharmaceutical industry will likely never be as competitive as some industries that more closely approximate perfect competition. Several factors, such as the patent protection and the price insulation for consumers, will necessarily limit the industry’s competitiveness. But that is not a bad thing. As Secretary Summers has pointed out, information-based companies need patent protection if they are going to spend heavily up front on research and development. Even so, it is possible that the pharmaceutical market could work better, especially if Congress and some of the regulatory bodies were to remove some of their restrictions and regulations.
Increasing Competition by Deregulation
If Congress is concerned about drug company prices and profits, the proper response is to adopt policies that encourage competition, not restrict it as price controls would do.
Indeed, some steps in this direction have already been taken. For example, in 1991 the FDA published regulations intended to accelerate the review of drugs targeting life-threatening illnesses. And the faster a drug can move through the process and hit the pharmacies, the more competitive the market will be.17
In addition, 1997 legislation that attempted to speed up the drug approval process and loosened restrictions for advertising has had a dramatic affect on increasing advertising over radio and television. Consumers are increasingly becoming familiar with prescription drug products and what they do. That’s important since a knowledgeable consumer and brand identification are necessary to a competitive market.
So while Congress has taken some steps in the right direction, there is much more it could do. For example:
(1) Reform Medical Savings Account legislation. As mentioned above, price insulation makes consumers indifferent to prices. For example, if a person’s prescription drug benefit requires a $20 copayment on a name brand drug, what difference does it make to the consumer if there is a price variation between two competing drugs? While some physicians encourage their patients to take the most cost-effective alternative, there is little reason for the patient to do so.
However, were Congress to reform the current Medical Savings Account (MSA) legislation by removing some of its restrictions, more people would choose MSAs over traditional insurance. For example, a recent Zogby America poll found that 82.1 percent of the respondents agreed that “all employers should have the option of offering their employees a medical savings account if they want.”18
Once more people had a high-deductible policy and had to pay for routine care and smaller expenses such as prescription drugs out of their MSA, they would be much more price sensitive. And once consumers begin to care about the price of drugs, the drug companies will have to begin to compete on price — or explain why paying more for a particular drug is a better value.
(2) Relax the FDA’s demand that new drugs prove themselves efficacious. According to Dixie Farley of the federal Food and Drug Administration (FDA):
“[T]he FDA’s decision whether to approve a new drug for marketing boils down to two questions: (1) Do the results of well-controlled studies provide substantial evidence of effectiveness?; and (2) Do the results show the product is safe under the conditions of use in the proposed labeling? Safe, in this context, means that the benefits of the drug appear to outweigh its risks.”19
Of course, comparing the cost versus the benefits of a drug can be very subjective, since different people differ in their willingness to take on risk. People also differ in their chemical makeup. A drug that is very effective for one person may not work for the next four and make the fifth ill.
As a result of the FDA’s requirement for new drugs to prove their efficacy, patients who could benefit from a new drug may wait for years — too long for some — before it becomes available. And when it finally does reach the market, they will pay a lot more for it than they should — and for many, a lot more than they can afford.
It wasn’t always that way. Until 1962 the federal government’s primary role was to protect patients from blatant fraud, not from themselves (that is, an informed decision to take a medication). However, the Kefauver-Harris Drug Amendments of 1962 attempted to ensure both the safety and efficacy of new drugs. Thus, drug companies not only had to prove that new drugs were safe, they had to prove they worked.
Kefauver-Harris may have been the most costly piece of regulatory legislation ever passed. Currently, moving a new drug from inception through the approval process takes eight to 10 years and costs $500 million to $600 million. If safety were the only thing the FDA monitored, it could take only $50 million and perhaps one or two years to get a new drug to patients.20
Imagine how much less expensive prescription drugs would be if the approval process cost a tenth of what it now costs. And the shorter approval time would mean that drug companies would have perhaps six to eight more years under their patents so that recouping their research costs could be spread out over a longer period of time.
Would eliminating the need to test new drugs for efficacy put patients at risk? Not necessarily. The current lengthy approval process doesn’t guarantee either safety or effectiveness. There are drugs that pass the FDA approval process that must be recalled because of adverse reactions. For example, both the anti-diabetes drug Rezulin and the antibiotic Trovan were FDA approved but were pulled after widespread use resulted in liver toxicity in some patients.21
Were the FDA to drop its demand for efficacy, but require strict physician oversight and the informed consent of patients, the approval process would move more quickly. As a result, more patients would have greater access to more new drugs, and drugs would cost less because the approval process would be so much shorter.
(3) Require only one clinical trial. Short of eliminating the requirement to prove efficacy, the FDA could make the approval process faster, smoother and cheaper. For example, the current standard is two clinical trials. The purpose of the second is to validate the first. The second trial must demonstrate equal or better outcomes. Although the FDA claims that often it does require only one trial, it usually asks for additional confirmation of the original trial’s findings, undermining the one-clinical-trial approach.
(4) Permit clinical markers to indicate a drug’s effectiveness. Once the clinical trials are done, researchers must put the outcomes information together in an effort to prove the new drug is effective. But why wait until the end of the lengthy clinical trial process? If a clinical marker — such as the size of a tumor in a cancer patient — is shrinking as a result of a new therapy, why not move to make that drug available then rather than at the end of the process?
(5) Allow greater freedom in altering the manufacturing process. When drug manufacturers alter their production process of a drug such as making changes in ingredient suppliers, processing methods or if they move production from one plant to another, they must obtain prior approval from the FDA. Although the FDA claims it has changed the process so that drug companies need only notify the agency, manufacturers still encounter delays and are forced to make numerous requests. Eliminating these encumbrances — which have little to do with the safety or efficacy of a drug — would reduce paperwork and administrative costs.
Creating a Prescription Drug Safety Net
In the midst of this political battle over a prescription drug benefit, there is a real public policy problem: ensuring that seniors have access to costly prescription drugs now and in the future. It is a problem that will grow more acute as the number of seniors swells and drug companies continue to develop new drugs that will make our health and lives better and more enjoyable.
Is there a way to provide for that need? Yes, but it needs to be a solution similar to the one free market proponents turned to for solving the problem of access to health insurance.
People sympathetic with government-run health care constantly try to reform the whole health insurance system so that sick people can join at any time for a reasonable price (the same thing they want to do with their prescription drug benefit). This destroys an insurance market because healthy people drop out, secure in the knowledge they can return if they get sick.
By contrast, free market advocates have thrown their support behind state-run high-risk pools for those who have been denied health insurance. Currently, 28 states have such programs. High-risk pools let the market work for some 98 percent of the people, while at the same time providing a safety net for those who need health insurance but can’t get it because of a medical condition.
Now apply this philosophy to a prescription drug benefit. Congress could create a catastrophic drug benefit plan that provides a safety net for seniors with very expensive drug bills. Both the Republican and Democratic plans already include a catastrophic element, though the Democrats only reluctantly added it in response to criticism.
Better yet, let the states manage the program, perhaps by their high-risk pool organizations (indeed, some states have already created prescription drug programs for poor seniors).
Set a cap of, say, $3,000 per senior — about five times what they spend annually, on average. Once the senior (or his supplemental insurance policy or Medicaid, etc.) spends $3,000, then the program would pay most or all of the additional costs. This solution would provide assistance only to the approximately 6 percent of seniors who spend more than $3,000 a year, and only in the year(s) they need help.22 Were the catastrophic deductible even higher, say, $5,000, it would affect an even smaller percentage.
Moreover it:
- Doesn’t create a new entitlement program;
- Would be a lot cheaper than what either the Republicans or Democrats are considering;
- Would encourage doctors and patients to choose the most effective therapy — drugs or surgery — without regard to which one is subsidized by Medicare and which one must be paid for out of pocket;
- Would keep the government out of the drug business — and out of most seniors’ medicine cabinets; and
- Has the benefit of creating only a safety net, not a hammock.
Finally, since private insurers offering drug coverage wouldn’t have to meet catastrophic costs anymore — only those up to $3,000 — they could lower their premiums, making standard coverage more affordable and more available.
Remember, fully two-thirds of seniors already have a prescription drug benefit, though some of their plans limit how much they pay. And many of those who don’t have prescription drug coverage are healthy and have chosen not to buy it.
Why would we add a new entitlement to a financially strapped Medicare program that would pay for drugs that many seniors could pay for out of pocket? Ideally, Congress should do a complete overhaul of Medicare that would introduce a prescription drug benefit. If Congress has to do something short of comprehensive reform, then let the prescription drug market work and create a program for those whom the market doesn’t work very well. What we need is a prescription drug safety net, not a new entitlement.
The Importance of Value.
Almost completely lost in the prescription drug debate is the role of value. In every other sector of the economy where consumers pay for what they want out of their own pocket, they look for value for their dollar. The pervasive rise of health insurance has almost totally removed the notion of value in health care decisions. Patients who pay only a fraction of the cost of health care, if they pay anything at all, seldom ask whether the treatment is worth the cost.
This problem has been exacerbated under Medicare since the program pays for some types of therapies, but not for others (i.e., prescription drugs). As a result, seniors may have chosen more expensive, less effective or more dangerous therapies simply because they were what Medicare was willing to pay for. Who knows the real cost — in money, in pain and suffering, and in lives — because of that perverse incentive?
The only way to return some sense of value and patient choice to Medicare is to provide some form of prescription drug benefit. A catastrophic prescription drug benefit would create a more level playing field between therapies. Since the care would be subsidized, seniors might still choose the more expensive therapy, but at least they wouldn’t be putting themselves in unnecessary risk just because they couldn’t afford one of their options.
Conclusion
If Congress and state legislators are serious about controlling drug prices, they should be removing restrictions from the pharmaceutical industry, as Congress did in 1997, to allow more competition. Given more competition, prices and profits would decline, but they would do so voluntarily. That is, the pharmaceutical manufactures themselves would look for ways to hold down costs as they tried to maintain their market share. There would be increasing pressure to develop more new drugs to compete with other profitable drugs and keep prices down in order to stay competitive.
There are two ways we can hold down drug prices: either externally or internally. When the government imposes price controls externally, it leads to reduced research and development, shortages and rationing — with Europe and Canada being the best examples. When drug companies voluntarily lower their prices in order to compete, they also look for new ways to get new products on the market faster.
Competition in a market relatively free of regulations, not price controls, is the best way to keep drug prices low. Educating patients about the benefit of the drugs they buy creates a sense of value for their money. And when consumers perceive they are receiving value for their drug dollars, no one would care what kind of profits the drug companies make.
Endnotes
- “Pharmaceutical Industry Profile 2000: Research for the Millennium,” Pharmaceutical Research and Manufacturers of America, Washington, D.C., March 2000, p. 113, Table 1. Some estimates of current research spending go as high as $26.4 billion. See Gardiner Harris, “Drug Firms, Stymied in the Lab, Become Marketing Machines,” Wall Street Journal, July 6, 2000.
- Lawrence H. Summers, “The New Wealth of Nations,” Remarks before the Hambrecht & Quist Technology Conference, San Francisco, California, May 10, 2000. Available at www. treas.gov.
- Ibid.
- Ibid.
- See Boston Consulting Group, “The Contribution of Pharmaceutical Comapnies: What’s at Stake for America,” September 1993. According to the study, the pre-tax cost of developing a drug in 1990 was $500 million, including the cost of research failures and interest on the investment.
- “Fortune One Thousand: Ranked within Industries,” Fortune, April 17, 2000, plus the annual editions since 1990.
- Patricia M. Danzon, “Price Comparisons for Pharmaceuticals: A Review of U.S. and Cross-National Studies,” April 1999.
- “Pharmaceutical Industry Profile 2000,” p. 58.
- Margaret Davis, et al., “Prescription Drug Coverage, Utilization, and Spending among Medicare Beneficiaries,” Health Affairs, Vol. 18, No. 1, January-February 1999; and Michael E. Gluck, “A Medicare Prescription Drug Benefit,” National Academy of Social Insurance, Medicare Brief No. 1, April 1999. Numbers do not add up to 65 because some seniors were classified in transitional coverage.
- The Consumer Expenditure Survey, conducted by the Bureau of Labor Statistics, estimates average annual expenditures to be about $637. See Merrill Matthews Jr., A Prescription for Disaster,” National Center for Policy Analysis, NCPA Brief Analysis No. 288, April 19, 1999.
- Charles Ornstein, “Seniors Fear Loss of HMOs,” Dallas Morning News, July 8,2000.
- See Stephen D, Moore, “In Drug-Cost Debate, Europe Offers U.S. a Telling Side Effect,” Wall Street Journal, July 21, 2000.
- Pharmaceutical Research and Manufacturers of America.
- Taren Grom, “Tuned In,” Med Ad News, October 1998.
- Ibid.
- Ibid.
- See “Milestones in U.S. Food and Drug Law History,” Food and Drug Administration, FDA Backgrounder, May 3, 1999.
- “82% voters want option to purchase medical savings accounts, new Zogby America survey shows,” Zogby International, July 25,000.
- Dixie Farley, “Benefit vs. Risk: How FDA Approves New Drugs,” FDA Consumer Special Report on New Drug Development in the United States, Food and Drug Administration, January 1995.
- William K. Summers and James Driscoll, “To Cut Drug Prices, Reform FDA,“ Wall Street Journal, June 21, 2000.
- Ibid.
- Martha H. Phillips, "A Primer on Medicare," The Concord Coalition, July 31, 2000, p. 42. Cited from National Academy of Social Insurance, 1999
